When blood sugar spirals out of control, the brain pays the price. A diabetic coma happens when blood glucose drops to a critical low or climbs to a dangerous high and the brain simply stops functioning. Not slows down. Stops. That's a medical emergency, and the clock starts the moment someone loses consciousness.
Key Takeaways
- A diabetic coma occurs when blood sugar hits an extreme high or low, causing full unconsciousness
- Three conditions lead to it. DKA, HHS, and severe hypoglycemia each carry different sugar levels and timelines
- It won't resolve without medical treatment. Full stop
- Fast treatment gives most people a full recovery; delay raises the risk of permanent brain damage
- Consistent blood sugar monitoring and proper nutrition are the strongest prevention tools you have
What Is a Diabetic Coma?
Here's what's actually happening in a diabetic coma. The brain runs almost entirely on glucose. Take that glucose away, or make the blood too acidic from ketone buildup, and the brain shuts down. The person goes unconscious and won't wake up no matter how loudly you call their name.
People in a diabetic coma are alive. Breathing. But completely unreachable without medical intervention.
Worth knowing. Some people discover they have diabetes for the first time during a diabetic coma. The condition doesn't only strike those with a known diagnosis.
Types of Diabetic Coma
Three distinct medical crises can push someone into a diabetic coma. Each takes a different path to get there.
Diabetic Ketoacidosis (DKA)
Most common in Type 1 diabetes. Without enough insulin, the body can't burn glucose, so it burns fat instead. Fat breakdown releases ketones into the bloodstream. Too many ketones and the blood turns acidic. The body starts failing from the inside out.
Diabetic coma sugar level in DKA sits above 250 mg/dL, but blood glucose alone doesn't tell the whole story. Ketone levels drive the real danger.
DKA builds over hours to a couple of days without treatment. Once unconsciousness sets in, things move fast. Hospital treatment with IV insulin and fluids typically brings most people around within 24 to 48 hours. The mortality rate runs between 0.2% and 2.5%. Survivable with quick care. Much worse with delay.
Hyperosmolar Hyperglycemic State (HHS)
Type 2 diabetes is where HHS does most of its damage, and it's a slow burn over days or even weeks. Blood sugar climbs to extraordinary heights without producing the ketones you'd see in DKA. The kidneys keep flushing glucose out through urine, and the body dries out from the inside.
The diabetic coma sugar level in HHS usually sits above 600 mg/dL. Cases have been documented above 1,000 mg/dL.
Because it sneaks up gradually, HHS often goes unrecognized until the person becomes confused, then unresponsive. That's a dangerous gap. The mortality rate reaches up to 20%, far higher than DKA, partly because HHS tends to hit older adults managing multiple health conditions and partly because it gets caught late.
Severe Hypoglycemia
No high blood sugar here. This one goes the other direction entirely. Blood glucose crashes below 40 mg/dL, and the brain loses its fuel source within minutes. Someone on insulin who takes too much, skips a meal, or exercises hard without adjusting their dose can go from feeling shaky to unconscious faster than most people expect.
This is exactly what people mean when they ask about diabetic coma vs insulin shock. Different name, same crisis. "Insulin shock" is the older term for a hypoglycemic coma. Glucagon or IV dextrose brings most people back quickly once they reach a hospital, but brain damage becomes a real risk if treatment gets delayed. The diabetic coma sugar level in severe hypoglycemia sits below 40 mg/dL.
Symptoms and Warning Signs
Catching the signs early is the difference between a close call and a catastrophe. They shift depending on whether blood sugar is high or low, and they get harder to miss as things escalate.
Early on, high blood sugar announces itself through relentless thirst, trips to the bathroom every hour, blurry vision, and bone-deep fatigue. DKA specifically adds fruity-smelling breath, caused by ketones building in the blood. Low blood sugar hits differently. Sudden shakiness, cold sweats, a heart rate that spikes, skin going pale, and hunger arriving out of nowhere.
Get closer to a coma and the signals change. Confusion sets in. Speaking becomes difficult. Severe hypoglycemia sometimes triggers seizures before unconsciousness arrives. HHS can produce hallucinations and partial vision loss. DKA brings rapid, deep breathing (called Kussmaul breathing) alongside worsening stomach pain. At this stage, waiting to see if things improve isn't a real option.
Complete unresponsiveness means the coma has arrived. Eyes closed. No reaction to voice or touch. No voluntary movement. Call 911 right then.
What Causes a Diabetic Coma?

Most diabetic comas don't come out of nowhere. There's almost always a traceable cause.
Skipping insulin ranks as the most common one. Even a single missed dose lets blood sugar climb, and DKA can develop from there. Illness makes everything harder to manage. A stomach bug or a urinary tract infection pushes the body to release stress hormones that drive blood sugar up, even in people who are normally well-controlled.
Taking too much insulin flips it the other direction. A miscalculated dose sends glucose crashing and severe hypoglycemia follows fast.
Eating inconsistently while on insulin sets up the dangerous swings. Skipping lunch isn't just inconvenient. On insulin, it can send blood glucose into a critical low. Consistent nutritional counseling helps people build eating habits that keep levels steady rather than volatile.
Drinking alcohol on an empty stomach carries real risk for anyone taking insulin. The liver gets busy metabolizing alcohol and stops releasing stored glucose, which sends blood sugar plummeting without warning.
What to Do if a Diabetic Coma Happens
The steps below need to happen in order. Sequence matters here.
- Call 911 first. Before anything else. Tell the dispatcher the person has diabetes so responders come prepared.
- Don't give food or liquids. An unconscious person can't swallow safely and will choke.
- Roll them onto their side. This keeps the airway clear if they vomit while waiting for the ambulance.
- Give glucagon if the cause is low blood sugar. A glucagon injection or nasal spray raises blood sugar temporarily. It buys time, not a resolution. Keep that 911 call active regardless.
- Check blood sugar if you have a glucometer. That number gives paramedics a head start the moment they arrive.
Diabetic Coma Treatment
All three types require hospital treatment. No exceptions.
For DKA, doctors start with IV fluids to reverse dehydration and correct electrolyte imbalances. Insulin goes in through the IV, pulling blood sugar down gradually while shutting off ketone production. If an infection triggered the episode, that gets addressed alongside everything else.
HHS needs massive fluid replacement because the dehydration runs deep. Insulin comes in carefully and slowly, since dropping blood sugar too fast creates its own complications. Potassium and sodium levels need close management throughout the process.
Severe hypoglycemia gets IV dextrose immediately. If bystanders gave glucagon before the ambulance arrived, doctors assess whether additional glucose support is needed and monitor closely for complications.
Diabetic coma recovery begins as soon as blood sugar stabilizes. Hypoglycemic comas often reverse within hours of treatment. DKA and HHS recovery takes one to several days in the hospital. The harder question of diabetic coma is how long before death has no fixed answer. It depends on the type, the person's overall health, and how fast treatment arrives. What holds true across all three types is simple. Every hour without treatment raises the risk of irreversible brain damage.
After discharge, individual health education helps patients and families understand medication adjustments, recognize early warning signs, and build a monitoring plan that actually sticks.
Prevention
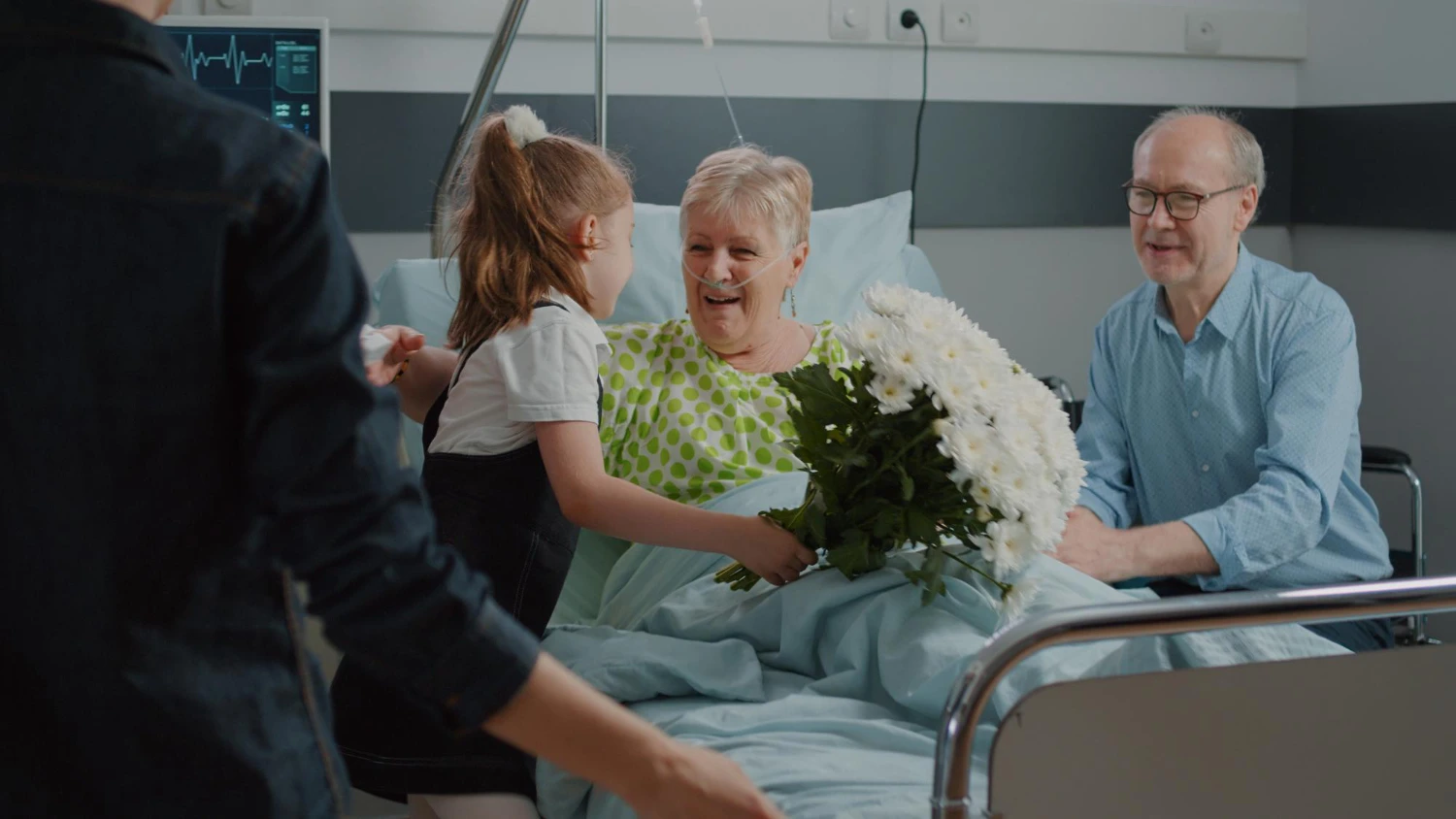
Good news: most diabetic comas are preventable. The fundamentals aren't complicated, just consistent.
Check blood sugar regularly. A CGM like a Dexcom G7 or FreeStyle Libre does this automatically, alerting you to dangerous dips and spikes around the clock. At minimum, check before meals, after exercise, and at bedtime.
Take medications exactly as prescribed. No adjusting insulin doses without a doctor's input, and no skipping on days you feel fine.
Eat on a regular schedule. Consistent meals prevent the swings that trigger crises. A nutritional counselor can map out a realistic eating plan built around your specific medication and lifestyle.
Plan ahead for sick days. Illness reshapes blood sugar behavior in ways that catch people off guard. Know in advance how often to check and at what point to call your doctor.
Wear a medical ID bracelet. If you're ever unresponsive, it tells first responders what they're dealing with before you can say a word.
Tell people around you where your glucagon kit lives. Family members, coworkers, close friends all need to know what to do. For people with more complex daily care needs, a personal care assistant can help manage medication schedules, meal preparation, and early warning detection day to day.
We're Here When It Gets Hard
Serious illness takes more than a prescription to manage. At LifeChoice Hospice and Palliative Care, our team provides individual health education, nutritional counseling, and personal care assistance for patients and families navigating complex health conditions.
Call 847-777-8888 anytime. We're available 24/7.














.webp)





